Quick Answer: Presentation anxiety relapse occurs when accumulated stress reactivates dormant fear patterns—a response that affects even highly experienced speakers. Neuroscientific evidence shows that anxiety memories remain encoded in your amygdala, and triggering events (job changes, higher stakes, trauma reminders) can reignite old responses. Recovery requires understanding the psychological mechanism behind relapse, systematic desensitisation, and rebuilding your nervous system’s threat response.
Jump to section:
The Day Priya’s Confidence Collapsed
Priya hadn’t felt anxious about presentations in seven years. She’d presented quarterly earnings to investors, led company-wide strategy sessions, pitched new initiatives to the board—all without a tremor. Then came the restructure.
Three months into a new role as VP of Operations, she was asked to present the quarterly performance review to an unfamiliar senior leadership team. The moment she stood up to present, her heart rate spiked. Her mouth went dry. The familiar dread she thought she’d left behind twelve years ago came flooding back.
“I thought I was done with this,” she told me in tears. “I don’t understand what’s happened. I’ve presented hundreds of times. Why is this coming back now?”
Priya isn’t alone. Presentation anxiety relapse is one of the most psychologically disorienting experiences for accomplished professionals—not because they lack competence, but because they’re facing a gap between their reality (I can do this) and their nervous system’s threat response (Danger. Not safe.). Understanding why this happens is the first step toward preventing it.
Ready to Stop This Cycle?
Presentation anxiety relapse isn’t a personal failure—it’s a neuroscientific reality that responds to targeted intervention. Conquer Speaking Fear teaches you the exact psychological and physiological techniques used by executive coaches to reset your nervous system and rebuild unshakeable speaking confidence.
Why Anxiety Returns Even When You’ve Conquered It
The psychological experience of relapse feels contradictory: you have objective evidence of competence (hundreds of successful presentations), yet your body and mind are reacting as though you’re in danger. This contradiction exists because anxiety and competence are processed by different systems in your brain.
When you overcome presentation anxiety through repeated exposure and success, you’re essentially building a new neural pathway—one that says “presenting is safe.” But the old pathway, the one created during your initial anxiety, doesn’t disappear. It remains dormant, encoded in your amygdala, ready to reactivate if the right conditions emerge.
Neuroscientist Joseph LeDoux calls this “retention of the original fear memory.” The brain doesn’t erase threat memories; it overwrites them with new, safer memories. When stress accumulates or a significant trigger appears, the original pathway can become active again—not because you’ve failed, but because your nervous system detects a mismatch between current demands and available resources.
This is particularly common among high-performing professionals for a specific reason: competence doesn’t always translate to psychological safety. You can be highly skilled at presenting and still feel unsafe doing it, especially if the stakes have increased, the audience has changed, or your personal circumstances have shifted.
Money Block #1: Transform Your Relationship with Speaking
Stop white-knuckling through presentations. Conquer Speaking Fear combines clinical hypnotherapy, NLP, and evidence-based breathing techniques to rewire how your nervous system responds to speaking situations.
- Reset your amygdala’s threat response in under 6 weeks
- Master physiological techniques that work during the presentation
- Build lasting confidence—not just for this presentation, but for your career
Created by a clinical hypnotherapist and NLP practitioner who overcame five years of severe presentation anxiety
The Neuroscience Behind Presentation Anxiety Relapse
To understand why relapse happens, you need to understand how your brain encodes fear. The amygdala—your brain’s threat-detection centre—is designed to be efficient, not accurate. When you experience presentation anxiety for the first time, your amygdala rapidly codes the presentation context (the room, the audience size, the silence when you’re speaking) as “threat.”
Each time you present without the catastrophe your brain predicted, new neural pathways form. These pathways are built through the prefrontal cortex—your reasoning brain—saying “This is safe. Nothing terrible happened.” This process is called “extinction learning,” and it’s the foundation of every anxiety recovery approach backed by evidence.
But here’s the critical detail: extinction learning doesn’t erase the original fear memory. Brain imaging studies show that the original amygdala encoding remains active, even after successful exposure therapy. What changes is that the prefrontal cortex learns to suppress or override the amygdala’s alarm signal.
Relapse occurs when something—stress, a significant life change, a triggering event—temporarily weakens the prefrontal cortex’s ability to override the amygdala. In that moment, the dormant fear pathway reactivates. It feels like you’re back to square one, but neurologically, you’re not. The old pathway is resurfacing, not because you lack competence, but because your nervous system’s regulation capacity has been temporarily compromised.
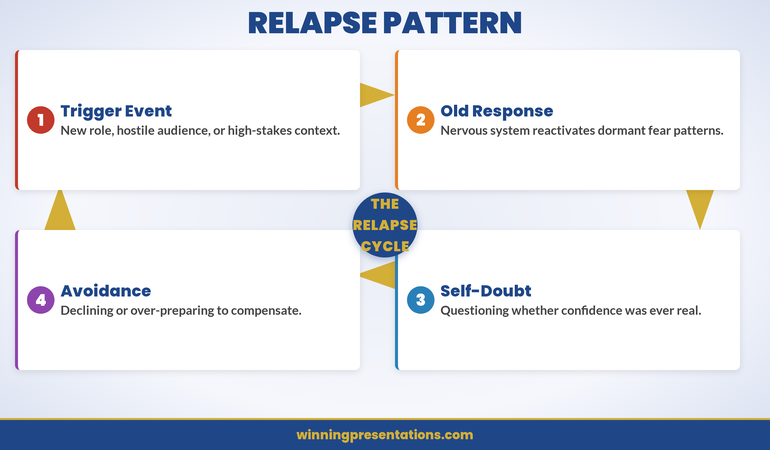
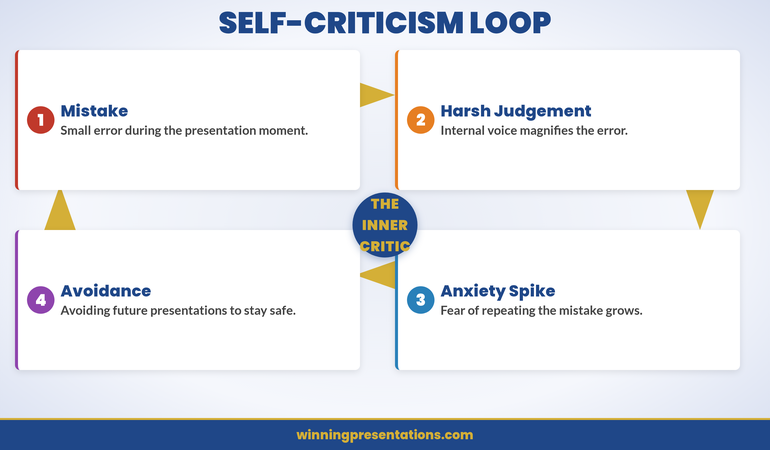
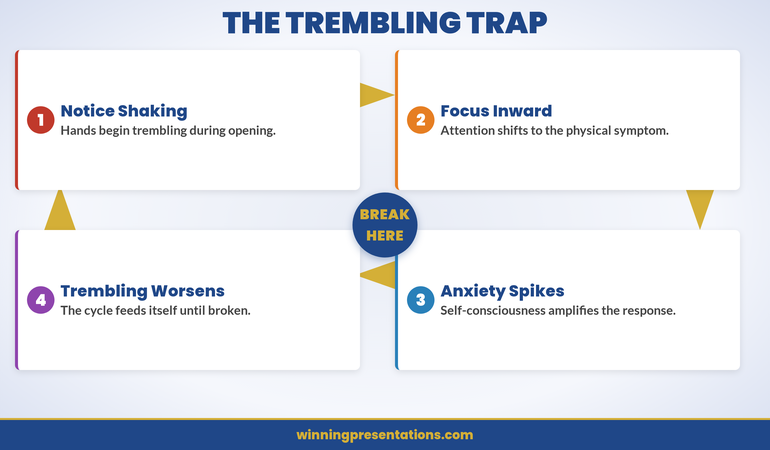
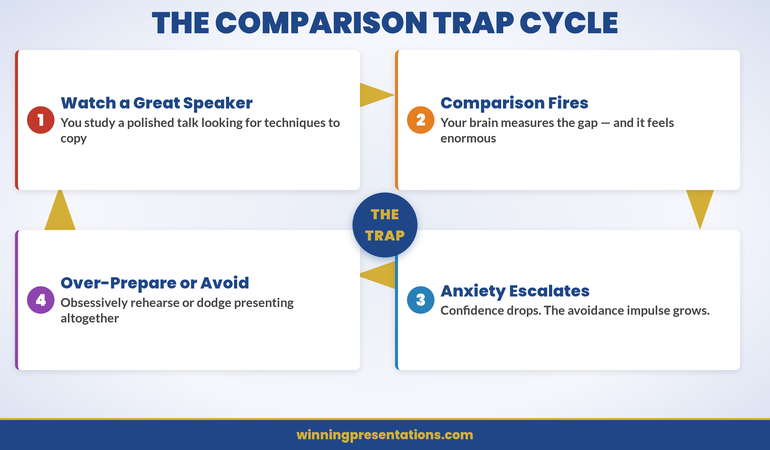
The four-stage relapse cycle: Trigger Event → Old Response → Self-Doubt → Avoidance.
The cycle shown above is what most professionals experience without realising it has a predictable shape. It begins with a Trigger Event — a new role, a hostile audience, or a high-stakes context that your nervous system hasn’t previously filed as “safe.” The trigger doesn’t need to be dramatic; it simply needs to be different enough from the conditions under which you built confidence that your amygdala registers a mismatch.
That mismatch activates the Old Response — the dormant fear pattern your nervous system retained from your original anxiety. Your heart rate spikes, your mouth dries, your hands shake. Neurologically, the prefrontal cortex’s override has been temporarily weakened, and the amygdala’s original threat encoding has resurfaced. This is not a new fear; it’s an old one reactivated under new conditions.
The old response generates Self-Doubt — the disorienting question of whether your confidence was ever real. This is the most psychologically damaging stage, because it reframes years of successful presenting as somehow fraudulent. “If I were really confident, this wouldn’t be happening.” But that logic is neurobiologically incorrect. Confidence and anxiety are processed by different systems; the return of one doesn’t invalidate the existence of the other.
Self-doubt then produces Avoidance — declining opportunities, over-preparing to compensate, or delegating presentations you would previously have welcomed. Avoidance feels like a rational response to the anxiety, but it’s the mechanism that entrenches relapse. Every presentation you avoid is a missed opportunity for your prefrontal cortex to reassert its override. The cycle feeds itself: avoidance weakens the safety pathways, which increases anxiety at the next presentation, which increases avoidance.
This distinction is psychologically crucial. If relapse meant “you haven’t actually recovered,” then recovery would be impossible after relapse. But if relapse means “your regulation capacity has been temporarily weakened,” then recovery is entirely possible—you simply need to rebuild regulation through the same mechanisms that worked before, under the new conditions.
Common Triggers That Reactivate Old Fear Patterns
Relapse rarely occurs randomly. Most often, it follows a recognisable trigger—a change in circumstances that signals to your nervous system that the safety conditions under which you built confidence have shifted.
Major life transitions are among the most common relapse triggers. A promotion, a job change, a move to a new organisation, even a new reporting relationship, can destabilise the “safety story” your nervous system has constructed. Priya’s relapse, for example, occurred during a restructure when she moved into a new role with unfamiliar stakeholders and higher visibility. The context had changed significantly, and her nervous system interpreted the new environment as requiring fresh threat assessment.
Increased stakes trigger relapse with remarkable consistency. You’ve presented a hundred times to your team without anxiety, but when you’re asked to present the same content to the board, your amygdala’s threat assessment suddenly shifts. The audience hasn’t changed your competence, but it has changed the stakes, and your nervous system reacts accordingly.
Trauma reminders are another powerful trigger. If your original anxiety was rooted in a specific traumatic event (a disastrous presentation that led to consequences, a humiliating question from an executive, a panic attack on stage), then situations that resemble that original trauma can reactivate the fear response. This is particularly true if the reminder is unexpected—your conscious mind may register safety, but your amygdala registers similarity, and similarity triggers threat.
Cumulative stress and sleep deprivation weaken the prefrontal cortex’s ability to regulate amygdala responses. You might present comfortably when well-rested and low-stress, but when you’re managing a crisis at work, dealing with personal challenges, or running on insufficient sleep, your nervous system’s resources are depleted. In this depleted state, old anxiety patterns can resurface, even with familiar presentation contexts.
Extended absence from presenting can trigger relapse because the safety pathways begin to weaken through disuse. If you’ve moved into a management role where presentations became less frequent, or if you took time off work, the extinction learning that protected you may gradually diminish. When you return to presenting, your nervous system is more reactive because the suppression pathways haven’t been recently reinforced.
Understanding your personal relapse triggers is essential, because it shifts the narrative from “I’ve failed” to “I’ve encountered a new condition that requires attention.” That shift—from shame to problem-solving—is where recovery begins.
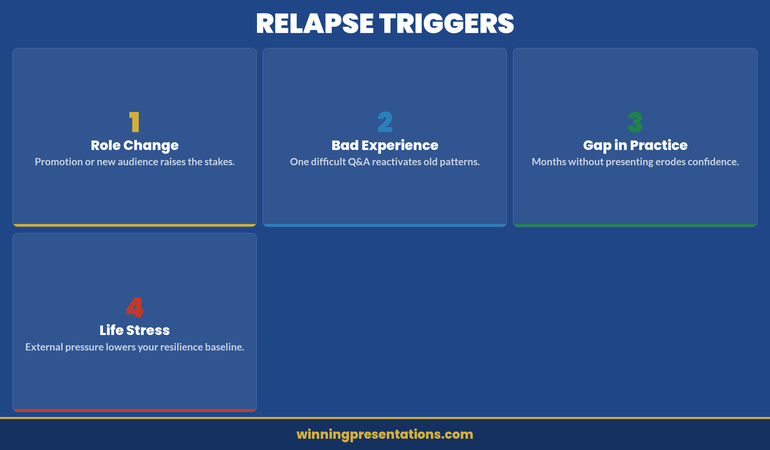
The four most common triggers that reactivate dormant presentation anxiety.
The four triggers shown above account for the vast majority of relapse cases. Role Change — a promotion, a lateral move, or a new audience — raises the stakes in ways your nervous system hasn’t previously processed as safe. Priya’s relapse followed exactly this pattern: same skill set, new context, and her amygdala treated the unfamiliar leadership team as a fresh threat requiring assessment.
Bad Experience — one difficult Q&A session, one hostile audience member, one moment of public stumbling — can reactivate old patterns with remarkable speed. The brain’s threat-detection system is designed to overweight negative experiences, because from an evolutionary standpoint, remembering danger is more important than remembering safety. A single bad experience can temporarily undo months of confidence-building if it resembles the original anxiety trigger closely enough.
Gap in Practice — months without presenting — erodes the extinction learning that protects you. Like any neural pathway, the safety connections between your prefrontal cortex and amygdala weaken through disuse. Professionals who move into roles with fewer presentations, or who take extended leave, often find that returning to presenting feels disproportionately difficult. The skill hasn’t diminished, but the nervous system’s confidence in that skill has.
Life Stress — external pressure from personal circumstances, workload, or health — lowers your resilience baseline. Your prefrontal cortex’s ability to regulate the amygdala’s alarm signal depends on available cognitive and emotional resources. When those resources are depleted by stress outside the presentation context, your nervous system’s capacity to maintain its override weakens. This is why relapse often coincides with periods of cumulative pressure, not with any specific presentation failure.
Have you noticed a pattern in when your presentation confidence shifts? Often it’s not about the presentations themselves, but about the context surrounding them.
Rebuilding Confidence After Relapse
Recovery from relapse follows the same neurobiological principles as initial anxiety recovery, but with one important adjustment: you already know recovery is possible because you’ve done it before. That knowledge is a significant advantage.
Step 1: Cease the shame response. The first barrier to recovery after relapse is shame—the feeling that you should have “stayed better” or that relapse indicates failure. Neuroscientifically, relapse is neither of these things. It’s a predictable consequence of how threat memories are encoded in the brain. Recognising this allows you to shift from emotional reactivity to strategic response.
Step 2: Identify the new safety threshold. In your initial recovery, you gradually exposed yourself to presentations to teach your nervous system that presenting was safe. After relapse, you need to identify what your nervous system now considers “safe.” This might be a smaller group, a lower-stakes presentation, or a familiar audience. Start there, not from the most challenging presentations.
Step 3: Use targeted desensitisation. Rather than waiting for naturally stressful presentations to rebuild confidence, create a structured exposure hierarchy. If relapse occurred when presenting to senior leadership, design a series of presentations at increasing visibility levels: first your immediate team, then a cross-functional group, then a larger audience, then senior stakeholders. Each successful presentation reinforces the prefrontal cortex’s override of the amygdala’s threat signal.
Step 4: Apply neurophysiological regulation techniques. Your body’s state influences your nervous system’s threat assessment. Before presentations, use specific breathing patterns, physical grounding, or gentle movement to shift your nervous system from sympathetic activation (fight-or-flight) to parasympathetic activation (rest-and-restore). This creates the physiological condition in which the prefrontal cortex can function optimally.
Step 5: Rebuild the safety story. Your original recovery was built on a “safety story”—a narrative your conscious and unconscious mind agreed on: “I can present safely.” After relapse, you need to update that story to integrate what triggered the relapse. The new story might be: “I can present safely, even when the stakes are higher” or “I can present safely in new contexts” or “I can present safely even when stressed.” This updated story, repeatedly reinforced through successful experience, becomes your new baseline.
Recovery after relapse typically takes 6-12 weeks, depending on the severity of the relapse and the strength of the triggering context. This is faster than initial recovery because your nervous system already has the neural pathways for safety—they simply need to be reactivated and strengthened.
If relapse has made you wonder whether you’re susceptible to chronic presentation anxiety, consider exploring what makes some professionals vulnerable to presentation trauma and others resilient. Understanding your own vulnerability factors helps you design recovery specifically for your neurobiology.
Want a structured system to rebuild your confidence? The Conquer Speaking Fear programme guides you through each of these steps using clinical hypnotherapy and NLP techniques specifically designed to work with your amygdala’s threat encoding.
Want the slides too?
Preparation reduces anxiety. The Executive Slide System (£39) includes confident-presenter templates designed to minimise preparation stress.
Recovery after relapse is faster than initial recovery—because the neural pathways already exist. What you need is a structured system to reactivate them. Conquer Speaking Fear combines clinical hypnotherapy, NLP, and evidence-based physiological techniques to reset your amygdala’s threat response and rebuild the safety story your nervous system needs. Not generic tips. Targeted intervention designed for professionals who’ve been confident before and need to get back there.
Maintenance: Preventing Future Relapse
Once you’ve rebuilt confidence, the question becomes: how do you prevent relapse from happening again? The answer lies in understanding relapse not as a risk to be eliminated, but as a challenge to be managed through ongoing nervous system maintenance.
Maintain regular exposure. The extinction learning that protects you from relapse is maintained through continued exposure. Professionals who present regularly (at least monthly) experience significantly lower relapse rates than those who present infrequently. If your role has shifted away from presenting, create opportunities to present anyway—volunteer for internal presentations, take on speaking opportunities outside work, or ensure you present at regular meetings even if not required. The goal is to keep the neural pathways for safety active and robust.
Track your stress baseline. Since relapse is often triggered by cumulative stress, maintain awareness of your overall stress levels and your nervous system’s capacity. During high-stress periods (project deadlines, personal challenges, significant life changes), take extra care with your presentation preparation and your nervous system regulation. This might mean more practice, more breathing work, or temporarily choosing lower-stakes presentations until stress levels normalise.
Update your safety story proactively. As you advance in your career and encounter new presentation contexts, proactively update your safety narrative. Rather than waiting for relapse to force an update, consciously expand your story: “I presented confidently to my team, so I can present confidently to the departmental directors. I presented to the directors confidently, so I can present confidently to the board.” This ongoing narrative expansion prevents the sudden context shifts that typically trigger relapse.
Use preventive nervous system regulation. You don’t need to wait until you’re anxious to use breathing, grounding, or movement techniques. Integrate them into your regular routine—daily practice strengthens your parasympathetic system’s capacity to regulate, meaning your nervous system is more resilient when stressors emerge.
Recognise early warning signs. Relapse rarely arrives without warning. Most people experience a period of increasing anxiety, restless sleep, or avoidant thinking in the weeks before relapse manifests. If you notice yourself avoiding presentation planning, thinking about presentations with unease, or noticing physical tension when presentations are scheduled, these are early warning signs. At this point, gentle intervention (increased nervous system regulation, a smaller practice presentation, reviewing your safety evidence) can prevent full relapse from developing.
Some professionals find that anxiety that doesn’t respond to standard techniques requires additional professional support. If relapse persists despite structured intervention, working with a therapist trained in exposure-based anxiety treatment can accelerate recovery.
Frequently Asked Questions
Can presentation anxiety relapse happen permanently?
No. Relapse is a resurgence of anxiety symptoms after a period of improvement, but it’s not a permanent condition. With targeted intervention, most professionals recover from relapse within 6-12 weeks. The critical difference between relapse and chronic anxiety is that relapse occurs in someone with existing neural pathways for safety, whereas chronic anxiety persists in someone without those pathways. Your previous recovery proves that your brain can learn safety—relapse is simply a recalibration, not a regression to baseline.
If I’ve had one relapse, am I at higher risk of future relapses?
Not necessarily. One relapse doesn’t predict future relapse risk. What does predict future relapse is unaddressed vulnerability factors—chronic stress, infrequent presentation practice, or unresolved trauma triggers. If you address these factors after relapse (through consistent presenting, stress management, and potentially professional support), your relapse risk returns to baseline. Many professionals experience one relapse in their career but never another, because they’ve learned to recognise their personal triggers.
Is relapse a sign that my original recovery wasn’t “real”?
Absolutely not. Relapse is a normal neurobiological phenomenon even after successful recovery. Your original recovery was real—it changed your brain, built new neural pathways, and gave you a period of genuine confidence. Relapse doesn’t erase that. What it does is reveal that anxiety recovery, like physical fitness, requires maintenance. You wouldn’t expect to run a 5K once and be fit forever; similarly, anxiety recovery requires ongoing attention to nervous system maintenance. The fact that you recovered once proves you can recover again, and usually faster.
The Path Forward
Presentation anxiety relapse is disorienting precisely because it contradicts your lived experience of confidence. But neuroscientifically, it’s entirely predictable and entirely recoverable. Your amygdala’s original threat encoding hasn’t been erased—it’s been overridden by years of safety evidence. When that override weakens under stress or significant context change, the old pathway resurfaces temporarily. But it’s temporary only if you treat it as a solvable problem rather than a permanent failure.
Recovery after relapse follows the same principles that got you here in the first place: gradual exposure, nervous system regulation, and a renewed commitment to the safety story your brain needs to hear.
Subscribe to The Winning Edge, the weekly executive briefing on presentation psychology and confidence-building techniques. Delivered every Thursday.
More in This Series
You’re reading Article 3 of today’s four-part exploration of presentation psychology for senior leaders. Dive deeper into related challenges:
- Article 1: Succession Planning Presentations — Managing stakeholder expectations when announcing leadership transitions.
- Article 2: Department Update Presentations — Communicating change clearly to mixed-seniority audiences.
- Article 4: Virtual Presentation Q&A Sessions — Mastering real-time interaction and follow-up handling.
Mary Beth Hazeldine is Owner & Managing Director of Winning Presentations. A qualified clinical hypnotherapist and NLP practitioner who overcame five years of severe presentation anxiety, she combines 24 years of corporate banking experience at JPMorgan Chase, PwC, Royal Bank of Scotland, and Commerzbank with evidence-based techniques for managing presentation fear.